Care Coordination
The Healthcare Journey
Overwhelms People

50% confused about healthcare & their plan
44% stop seeking care for a needed service
24% of physician services duplicated
Care Coordinators Completely Replace Member Services
& Guide Your People Through the Healthcare Maze
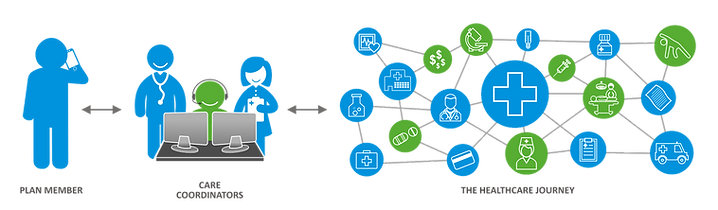
Move beyond insurance plan member services and a separate plan advocacy/ concierge vendor to supplement it. Completely replace them both with Care Coordinators. Our Care Coordination approach is a single, dedicated pod of about 25 professionals screened for empathy, highly trained & using patented technology. They include nurses and plan advocates on the direct member facing team. These health care warriors become the single point of contact for plan members and their medical providers.
Care Coordination Means Concierge Level of Service for Everyone
Care Coordinators provide:
-
Patient Advocacy
-
Care Management
-
Nurse Coaching
-
Regular Plan Services
Examples:
-
Find a top quality in-network provider
-
Make an appointment
-
Have test results forwarded to a doctor
-
Proactively provide post-surgical instructions to members
Stats:
-
35% of their calls are outbound
-
53% of their contacts are to providers on behalf of members
-
7.5 minute ave. call time with member vs. 1.5 minute industry ave.
Key Features of The Pod
Nurses on Member Facing Team
Plan Advocate Service
Totally Integrated
-
1 Co-Located Team
-
1 Phone Number
-
1 Tech Platform
With nearly 20 years of research and application, our Care Coordinators have established systems that tell them when to reach healthcare consumers. On average, they engage with members 56 days earlier than other models. In order to help them get better care and avoid wasting time and healthcare dollars.
Real-Time InterceptTM
A 56-Day Advantage
Great Things Happen With
Care Coordination
Data represents average results of entire book of Care Coordinator business including over 1 million plan members and is validated annually with formal reporting by a national actuarial firm. Fix Healthcare provides this report at point of presentation.
